[ad_1]
WASHINGTON (AP) – Take a look at the baby UTI from all US hospitals: you will see sick and premature newborns covered with wired monitors tearing fragile skin and preventing parents from cuddling their children.
Researchers have now created tiny skin-type wireless sensors that could eventually cut these cords.
"This need was so compelling," said John Rogers, a bio-engineer at Northwestern University, who led the development of the sensors. "Without the wires, it's much easier for parents, especially mothers, to interact and hold on to their baby."
Nearly 300,000 newborns in the US are in neonatal intensive care units each year because they are born prematurely or have serious health problems. It is essential to monitor their heart rate and other vital signs so that doctors and nurses can quickly detect if their youngest patients are in difficulty.
But today, it means sticky electrodes attached by wires to a variety of beeper monitors that surround the incubator. The nest of threads prevents skin-to-skin contact with a parent known to help premature babies develop, let alone shake a baby or nurse their baby, said Dr. Amy Paller, a North West pediatric dermatologist.
And no matter how carefully doctors and nurses remove electrodes, premature babies whose skin is not fully developed are prone to injury and scarring.
Wireless use in the NICU is much more difficult than, for example, measuring the heart rate of a jogger with a FitBit.
First, the Rogers team has developed ultra-thin, flexible silicone sensors that move like a skin and attach themselves without any strong adhesive.
The researchers then integrated the sensors with spring-loaded electronic components, flexible as the body moves, impervious and made of materials that, unlike current NICU monitors, do not interfere with X-rays or MRIs.
And the key to being lightweight, they do not need batteries. Under the bed mattress is a transmitter that charges wireless sensors in the same way as some smartphone chargers – while simultaneously transmitting all sensor measurements to the hospital computers.
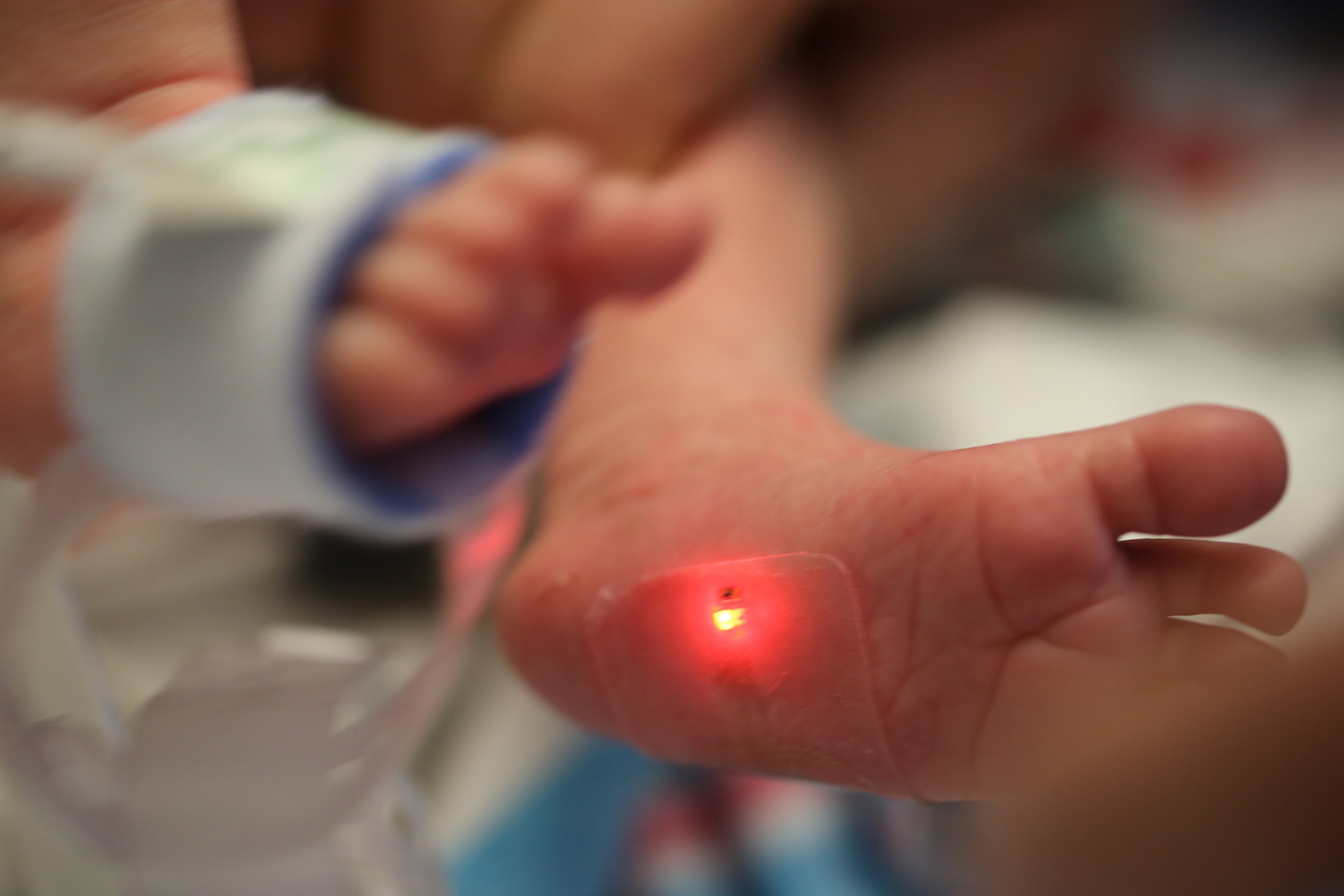
To replace several monitors today, just two wireless sensors – one for the chest or back and one to protect the foot – work together. For example, the upper sensor measures cardiac activity, while the foot sensor uses light to measure oxygen levels in the blood. The time it takes for a heartbeat to reach the foot is blood pressure, Rogers said – no armband is needed.
What is their reliability? The researchers placed wireless sensors on the bodies of 20 babies in the North West affiliated NICUs, who also benefited from normal wired surveillance. Wireless sensors have also worked well, Rogers and Paller reported Thursday in the journal Science.
"This is a promising technology that could eliminate the sensors to stick," said Dr. Rosemary Higgins, a neonatologist at the National Institute of Child Health and Human Development, who did not participate in the research.
Studies are continuing and Rogers said the sensors were used on about 80 babies with similar results and no signs of skin problems.
"It's really incredible," said Theodora Flores, as she held one of her binoculars, Genesis, at Ann & Robert H. Lurie Hospital in Chicago this week. Genesis is part of the wireless tests and the new mom said that fewer wires meant, "I can move freely with her a little more."
Much more testing is needed for wireless sensor approval by the Food and Drug Administration.
But Rogers said the biggest need is for developing countries that can not afford today's wired surveillance, even for pre-enemies. He estimates that the new sensors could be manufactured for about 10 to 15 dollars. With funding from the Bill and Melinda Gates Foundation and Save the Children, Rogers is preparing for a pilot test of wireless sensors in Zambia in April, with the goal of testing up to 20,000 sensors in India. Pakistan and Zambia by the end of the year.
The technology "has a significant potential impact on surveillance practices around the world and can give many newborns a fairer chance to survive," said Dr. Ruth Guinsburg of the Federal University of Sao Paulo in Brazil in a commentary published in Science.
___
AP video reporter Teresa Crawford has contributed to the story from Chicago.
The Associated Press Science & Science Department is supported by the Howard Hughes Medical Institute's Department of Science Education. The AP is solely responsible for all content.
[ad_2]
Source link