[ad_1]
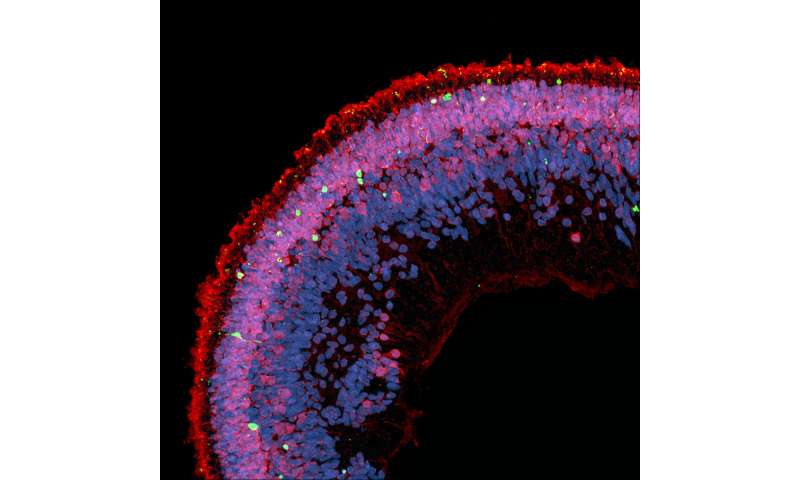
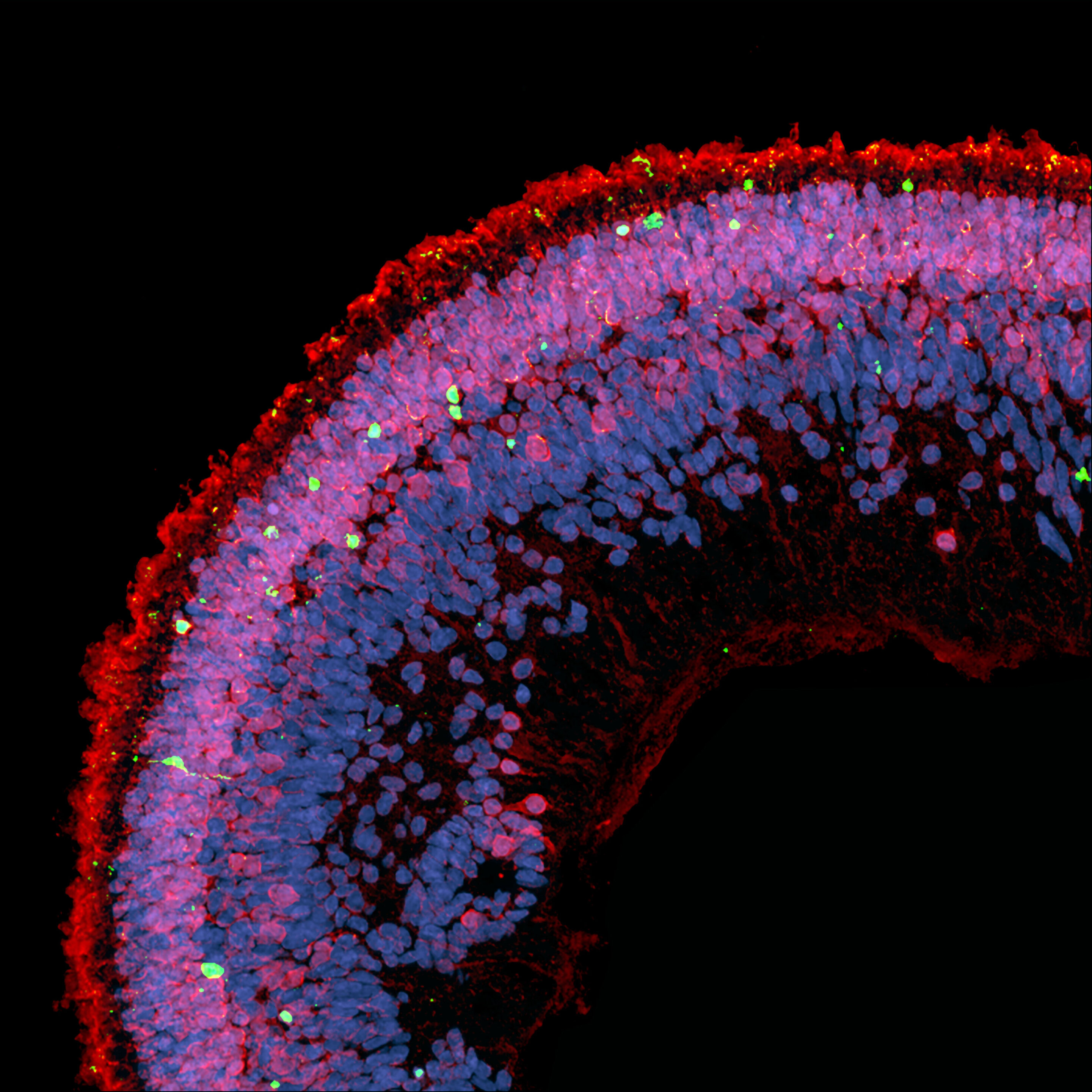
Cell death (in green) is observed in the cross section of a retinal organoid exposed to deoxysphingolipids. The photoreceptors appear in red on this image, the nuclei of the cells in blue. Credit: (c) Lowy / Kevin Eade Medical Research Institute
Scientists at the Lowy Medical Research Institute (LMRI) have discovered one of the causes of a progressive and debilitating eye disease called macular telangiectasia type 2 (MacTel). The work, which uses genetic, clinical and biochemical studies, has implications for other eye diseases of the retina, as well as for peripheral neuropathies.
"This is a major breakthrough not only for MacTel research, but also for eye, neurological and metabolic research," said Martin Friedlander, president of LMRI, Scripps Research professor, and lead author. with Christian Metallo, associate professor. at the University of California, San Diego and Paul Bernstein, professor at the Faculty of Medicine at the University of Utah. "This discovery was made possible only through a global network of talented doctors, scientists and patients collaborating with the generous support of enlightened philanthropists, the Lowys."
The research was published by the New England Journal of Medicine September 11, 2019.
Globally, it is estimated that MacTel affects about 2 million people, with symptoms usually appearing in the fourth and fifth decades of life. With retinal disease, a light-sensitive tissue located at the back of the eye, MacTel causes progressive deterioration of central vision in affected individuals, interfering with critical tasks such as reading and reading. conduct. There is currently no treatment for the disease.
Over the last 15 years, a group of scientists have been part of a highly focused international effort to find the cause of the disease and to develop effective treatments. Early efforts to use genetics to determine the cause have been frustrated by the association of the disease with a multitude of genes.
However, a single multi-faceted approach involving networks of patients and scientists, using not only genetics but also metabolomics, suggested that the disease was associated with low levels of serine blood. Serine is an amino acid used in many body pathways, but that, until now, had no effect on macular health.
In this article, LMRI researchers show that low serine levels in MacTel patients lead to an accumulation of toxic lipids, deoxysphingolipids, which cause photoreceptor cell death.
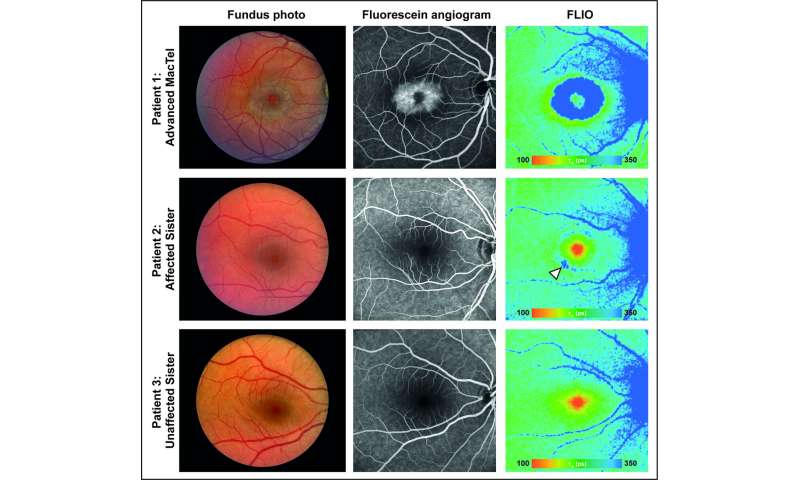
Multimodal imaging of three members of a family registered at the Center for MacTel Genetics of Utah is presented. Patient 1 shows signs of advanced MacTel in all imaging modalities; This is evident in the FLIO image by the blue central ring. The second patient, his sister, carries the mutated gene for MacTel, but his clinical imaging is unremarkable. Its FLIO image is the only modality that shows the first signs of MacTel (blue ring, see arrow). The third patient, another sister, does not carry the mutation of the MacTel gene and her imaging is normal. Credit: Lydia Sauer, MD
One clue that led to this discovery comes from a family comprising two people with both MacTel and a rare peripheral neuropathy, an inherited sensory and autonomic neuropathy (HSAN1), known to be caused by toxic deoxysphingolipids. The clinicians then conducted extensive eye examinations on a group of 13 HSAN1 patients and discovered that the majority of them also had MacTel.
"Deoxysphingolipids are toxic to neurons in other parts of the body, but no one knows if these lipids also play a role in eye diseases," said Marin Gantner, a scientist at LMRI and co-lead author of the paper with LMRI scientist Kevin Eade and UC Martina Wallace, postdoctoral fellow in San Diego. "Thanks to clues provided by MacTel and HSAN1 patients, we hypothesized that the low serine observed in MacTel patients could be at the origin of the body's formation of toxic lipids that damage the eye. "
Biochemically, that made sense. If serine levels are low, the enzyme responsible for the production of sphingolipids will use alanine instead, which will result in the production of deoxysphingolipids. The scientists extended their research to a large population of MacTel patients without HSAN1 and found that low serine in MacTel patients correlated with elevated levels of deoxysphingolipids. Researchers confirmed in mice that a low serine resulted in elevated levels of deoxysphingolipids in the blood, retina and peripheral nerves. This affected the sensory system of mice, reducing peripheral and retinal nerve function.
"In this case, a single biochemical mechanism causes eye and peripheral nervous system disease," Friedlander said. "We believe that it is an example of a new class of neurodegenerative diseases that we call" serineopathy "and that we could apply to more common metabolic and neurological disorders."
By bringing the research back to humans, scientists used human-induced pluripotent stem cell-based retinal organelles (iPSCs) to confirm that deoxysphingolipids are toxic to human retinal tissues.
"Recent advances in stem cell research have allowed us to make human retinal tissues called retinal organoids in the lab, retinal organoids that mimic the human retina," said Eade. "They allow us to study the cause of diseases of the retina and test the effect of drugs directly on the human retina."
The group found that the addition of fenofibrate, a prescription cholesterol-lowering drug, to retinal organelles exposed to deoxysphingolipids protects from photoreceptor cell death. Fenofibrate has been shown to stimulate degradation of deoxysphingolipids.
The unique LMRI research model is at the center of these discoveries. The Institute brings together a highly scientific group of scientists and clinicians from around the world and facilitates the exchange of information through regular meetings. Patient-centered research is at the heart of the model. The institute supports a MacTel patient registry and coordinates access to the patient's derived tissues for research. The Lowy Medical Research Institute builds on the generosity of the Lowy family and shows how philanthropy can advance research on rare diseases.
The next steps in the research are to discover the extent of the role of deoxysphingolipids in macular disease and to characterize the pathways that lead to high levels of deoxysphingolipids in MacTel.
The first genetic discoveries worldwide indicate a risk of blindness
Serine and lipid metabolism in macular disease and peripheral neuropathy New England Journal of Medicine (2019).
Provided by
Lowy Medical Research Institute
Quote:
Scientists find the cause of a disabling eye disease (September 11, 2019)
recovered on September 11, 2019
on https://medicalxpress.com/news/2019-09-scientists-debilitating-eye-disease.html
This document is subject to copyright. Apart from any fair use for study or private research purposes, no
part may be reproduced without written permission. Content is provided for information only.
[ad_2]
Source link