
[ad_1]

Photographer: Akos Stiller / Bloomberg
Photographer: Akos Stiller / Bloomberg
The road to eliminating Covid-19 is long and paved with uncertainties. Many countries rely on vaccines to create sufficient immunity in their populations so that SARS-CoV-2 is not able to find people who are likely to infect, which slows down and eventually stops the transmission of the coronavirus. But even with the deployment of highly effective vaccines, immunization coverage might not reach this level – the so-called herd immunity threshold – soon. On the one hand, it is does not know what level of immunity is required and whether vaccines will be powerful enough to do it. There is also the threat of emerging variants of coronavirus that may weaken the effectiveness of immunizations.
1. Can Covid-19 be eradicated?
No, so far only one human disease – smallpox – has been officially eradicated; that is, reduced to zero cases and stay there long-term without continued intervention measures. Smallpox was eradicated thanks to a very effective vaccine and the fact that humans are the only mammals to naturally susceptible to infection with smallpox virus which causes disfiguring, sometimes fatal disease. Humans are the only known reservoir of poliovirus, but it is still spreading a few countries causing crippling diseases despite widespread use of effective vaccines and a 32-year-old global eradication effort. SARS-CoV-2 is believed to persist in horseshoe-shaped nature bats, and is known to infect mink, cats, gorillas and other animals. To eliminate the virus, it would have to be banned from all susceptible species, which is not feasible. In countries that have succeeded in suppressing cases of Covid-19, disease elimination has been proposed instead.
2. What is elimination?
It was when efforts to suppress an epidemic resulted in zero new cases of disease or infection in a defined area over an extended period. There is no official definition of how long this should last. One proposal is to do it 28 days, corresponding to twice as long as the outer range of the SARS-CoV-2 incubation period – the time between infection and symptom onset. Some countries, like New Zealand, have not recorded any new cases for extended periods of time thanks to border closures, lockdowns and the diligent detection and isolation of cases. during a pandemic, which is an epidemic of a new infection across continents, supporting the elimination of any infectious disease nationwide is difficult, if not impossible, due to the threat of reintroduction of the virus into the country by infected international travelers.
3. Will the vaccines eliminate Covid-19?
It’s hard to say. We don’t know what a proportion of the population must be immune to keep the coronavirus from circulating, or if even the strongest vaccines will be able to stop it from spreading. One study estimated that to stop transmission, 55% to 82% of the population would need to be immunized, which can be achieved either by recovering from infection or by vaccination. However, collective immunity was not reached in Manaus, the capital of the state of Amazonas in Brazil, even after around 76% of the population infected. Still, there is reason to believe that mass inoculations will have a more potent effect, as vaccines appear to elicit stronger and longer lasting protection than a previous infection.
4. How effective will the vaccines be?
There is good evidence that the shots made by Pfizer Inc.-BioNTech SE and Moderna Inc. is very effective – up to 95% – at preventing recipients from developing Covid-19 on its own. However, no data has been published on their ability to prevent people from developing asymptomatic infections or passing the virus on to others. The gold standard in vaccinology is to stop infection as well as disease by providing what is called sterilizing immunity. But this is not always realized. The measles vaccine, for example, prevents infection so that vaccinated people do not spread the virus, while the vaccine for whooping cough protects well against serious disease, but is less effective at stopping infection. Encouragingly, a The study of Moderna’s Covid vaccine in monkeys suggested that it would reduce, if not completely prevent, transmission of the virus. Clinical trials using AstraZeneca Plc vaccine says it may be less than 60% effective in stopping infections – making herd immunity unlikely even if everyone in a population has received two doses.
5. How do virus variants come into play?
Researchers investigated the ability of antibodies in the blood of recovered Covid-19 patients to block the new, rapidly spreading B.1.1.7, 501Y.V2 and P.1 variants first reported in the UK , South Africa and Brazil. Some research has indicated that these strains may escape the immune protection offered by natural infection. Scientists have warned that laboratory studies are only indicative and there is no evidence that this is actually happening in the community, or that the antibodies generated by the vaccine will be less effective against the new strain.
6. Should Covid-19 vaccines prevent infection to stop cases?
No. Vaccines you don’t have to be perfect to benefit from public health benefit. New Zealand Vaccinologist Helen Petousis-Harris cites rotavirus and chickenpox as examples of diseases that have been “virtually eliminated with the help of vaccines that are very effective at preventing serious disease, good enough to prevent any disease, but which do not completely prevent disease. infection in everyone. Since SARS-CoV-2 is spread through respiratory particles in the throat and nose of an infected person, a vaccine that reduces the amount of virus in the airways or reduces the frequency of an infected person’s cough may decrease the likelihood of its transmission to others and reduce the effective reproduction number (Re), which is the average number of new infections estimated to be from a single case. Mike Ryan, Head of The World Health Organization’s emergency program told reporters on January 25 that instead of focusing on eliminating SARS-CoV-2, success should be seen as “reducing the capacity of this. virus to kill, to put people to the hospital, to destroy our economic and social lives. “
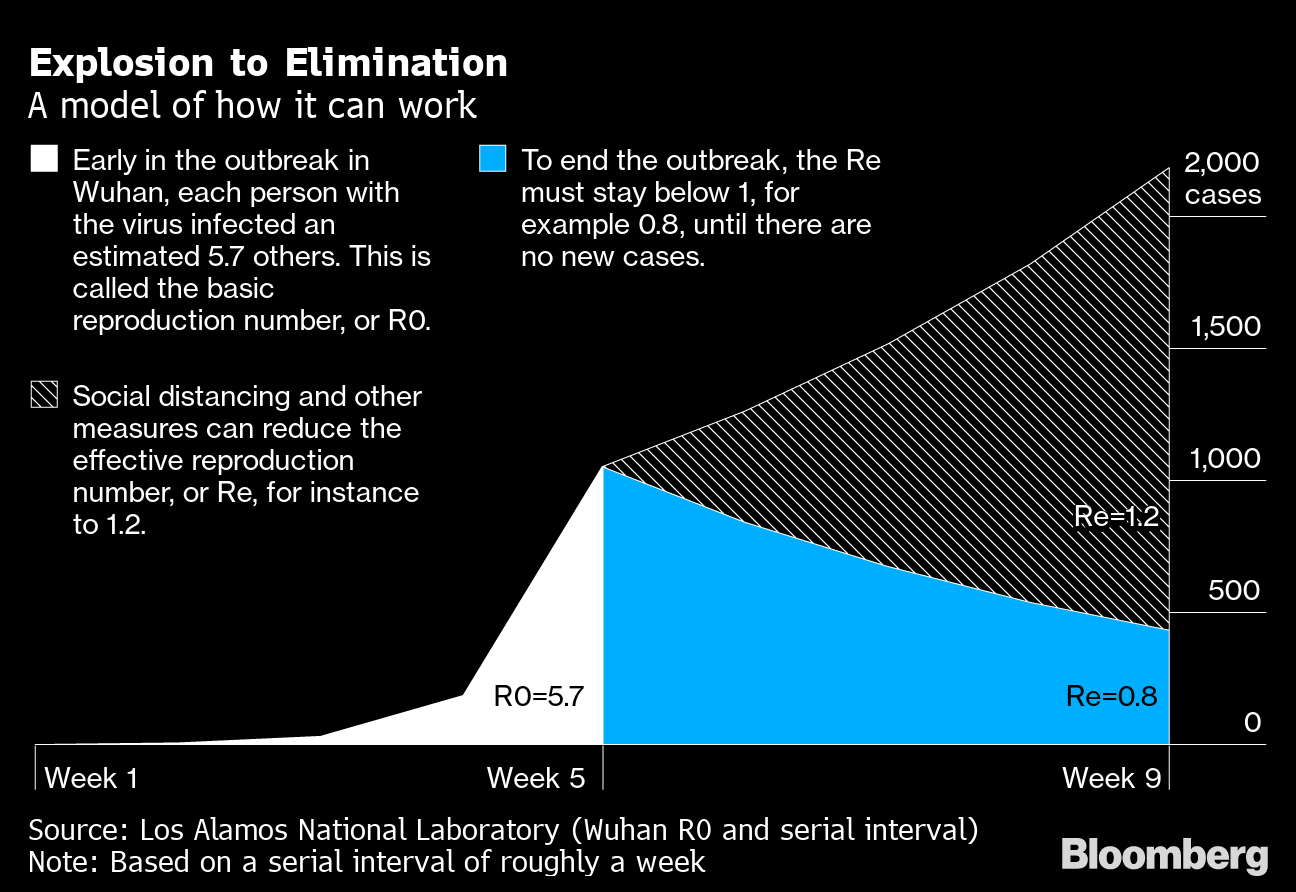
Elimination explosion
An operating model
Source: Los Alamos National Laboratory (Wuhan R0 and serial interval)
7. What if Covid-19 is not eliminated?
David Heymann, Chairman of the WHO Strategic and Technical Advisory Group on Infectious Risks, warned in late 2020, “It seems the fate of SARS-CoV-2 is to become endemic.” Endemic viruses circulate constantly in the community, often causing periodic spikes when disease characteristics and human behaviors favor transmission. Examples include norovirus, the notorious cause of gastroenteritis on cruise ships, and the myriad of viruses, four of which coronaviruses, which cause colds, especially during the winter.
8. What could be the implications?
It’s unclear how things will turn out, but researchers have started to develop scenarios. People who survived Covid-19 and those vaccinated against it will likely be protected against disease for a while. It is likely that a new exposure to the virus or a booster shot of the vaccine strengthen their protection. As more and more people develop immunity in this way, the virus will find those who are not yet, as long as herd immunity is not established to protect them. This will mean that people who cannot get the vaccine – because their immune system is compromised, or they have allergies to the ingredients in the vaccine, or they are too young (none of the vaccines allowed in Western countries have been approved. for children) – will remain vulnerable. Some scientists have predicted that once the endemic phase is reached and primary exposure to the virus in childhood, SARS-CoV-2 could be not more virulent than the common cold.
The reference shelf
- Devi Sridhar and Deepti Gurdasani of the University of Edinburgh detail the tough lessons from a largely uncontrolled Covid-19 outbreak in Manaus, Brazil.
- Anita Heywood and Raina MacIntyre from the University of New South Wales explain the eradication, elimination and suppression of the disease, and what elimination of Covid-19 would look like. MacIntyre also presents principles of vaccination programs for the fight against Covid-19.
- Related QuickTakes on How reluctance to vaccination threatens to delay the end of the pandemic, why delaying the second injection of a Covid-19 vaccine is complicated, why the mutated variants are so disturbing, how the coronavirus is transmitted on vaccine deployment, if you can be forced to get vaccinated, coronavirus treatments and unanswered questions about the virus.
– With the help of Alisa Odenheimer
[ad_2]
Source link