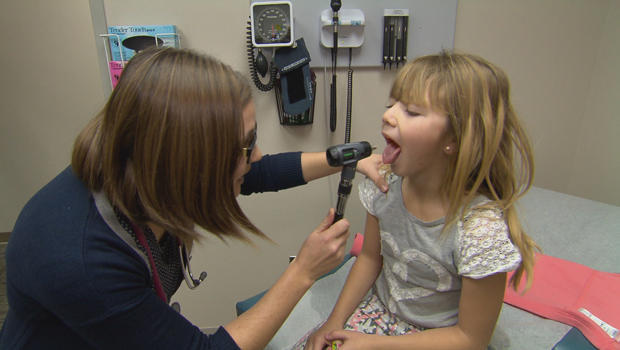[ad_1]
Tonopah, Nevada, is as isolated as possible: 200 miles south of Reno, 200 miles north of Las Vegas, with a road at the entrance or exit. But for those who call home, this picturesque spot in the desert has everything you need.
Emmy Merrow was not afraid of living in such an isolated place: "There was a shop and a gas station, and I was fine!" she laughed.
Merrow lived here for four years. She has a two-and-a-half year old daughter, Aleyna, and a newborn daughter, Kinzley.
They moved here when her husband received an excellent job offer from the sheriff's department. But six weeks before discovering that she was pregnant with Aleyna, she also discovered that the troubled Hospital of Tonopah, her only hospital, was definitely closing its doors.
"I'm frustrated, I'm angry, I'm crying, I'm angry because we would live less than a kilometer from a hospital," she said.
CBS News
It was all the more worrying that shortly after her birth, Aleyna was diagnosed with Dravet syndrome, a form of catastrophic epilepsy. "She's like any other typical child, and our day is like any other day except when she has epileptic seizures," said Merrow.
"And how much does she have a day?" asked correspondent Lee Cowan.
"She's about 400 now."
"So, is there anyone at a reasonable distance who can help?
"No."
When the seizures are severe enough, every six weeks or so, Merrow must rush mad and desolate to the nearest hospital on the California border, a hundred miles away.
She will never forget the first time she had to do it: "It was in the middle of the night, so it was dark and I could not see it. So I often stopped to check that she was fine. breathe again. "
"It must have been terrifying," Cowan said.
"Yes, I've been sobbing all the way in. It's the worst feeling in the world."
Elaine Minges also lives in Tonopah. She came here with her husband, Curt, for a well-paid job at the nearby solar plant, and thought that they would retire here one day. "We knew there was a hospital here and there were a few doctors, and we felt comfortable at that time," Minges said.
But after the closure of the hospital, everything changed. "They closed the doors and it was over," she said.
"And they did not warn you?"
There were rumors, she said, but "we thought no, it would not happen, it will not happen, look, we're in the middle of nowhere!"
Curt, who was suffering from diabetes, tried not to think about it until one night he suddenly became very sick. Minges remembered: "He woke up and I thought he was having a heart attack, he was out of breath, he tried to get up, but he was too sick."
He was suffering from a serious complication of diabetes. It's a disease that can normally survive with fast medical care, but in this case, you had to take a helicopter. "That night, the helicopter was out 45 minutes before he could get to the airport and, by that time, he went into cardiac arrest."
Cowan asked, "If the hospital here had been opened, would that have saved your husband?"
"I would like to think so, yes."
It is a sinister story that is repeated throughout the country.
Since 2010, 99 rural hospitals like Tonopah have closed down; it's almost one a month.
"By and large, about half of rural hospitals lose money every year," said Mark Holmes, professor of health policy and management at the University of North Carolina, who studies the decline. for more than a decade.
Cowan asked, "Is there an end in sight?"
"Whenever I said," I think we are going through the worst, "we were surprised," replied Holmes. "You must always ask yourself, who is the next?"
A representative sample from across America now faces the very real risk of not having to turn to a local hospital. The causes are varied; the population in some of these cities has shrunk to a size that can no longer support a hospital.
In others, hospitals are mismanaged or end up as table scraps in mega-mergers. The Medicaid expansion would have helped some stay open, says Holmes, but not all, and despite that, reimbursement rates are often too low for hospitals to break even. Whatever the cause, the impact on the community is almost always the same:
"The hospital is closing, the emergency rooms are drying up, all the other services that have been added – home care, pharmacy, hospice, EMS – have also left the city and now there is a medical desert", declared Holmes.
CBS News
This is exactly what worries the people of Pauls Valley, Oklahoma. The city, located about 100 kilometers south of Oklahoma City, has only one hospital, but the previous management company went bankrupt.
The city brought Frank Avignone to save him. During Cowan's visit, Avignone was working on the phone to find a generous donor: "I have 130 employees here and I will have to tell them that they have no future," did he declare.
"It's literally day-to-day for this hospital," Cowan asked.
"It's minute by minute," he replied.
"How much money do you have at the bank right now?
"About $ 7,000."
"What brings you to where?"
"The next 15 minutes – I mean, it's not enough to really make a difference."
City dwellers rallied, especially those who have been treated here, like Susanne Blake. She and her husband spent half of their savings on retirement – a bet that made sense to them. "We were seduced by everything we should give, because he said," Well, without a hospital, we do not have to worry about such a long retreat! ", She laughed.
The employees were just as passionate. Linda Rutledge, who has been working in the hospital cafeteria for nearly 20 years, has cooked more than a thousand cookies – a bake sale with a lot to gain.
When asked what would happen if the hospital were to close, Rutledge responded, "I'm going to cry, that just can not happen."
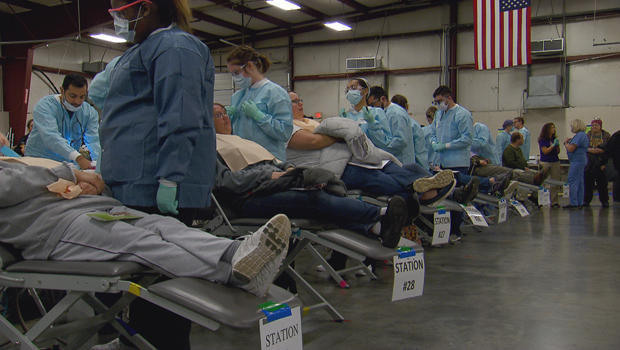
But that can happen. And last year, in response to the need for medical care, a large, free clinic was launched in an exhibition park in Gray, Tennessee, created by a non-profit organization called Remote Area Medical, created in Toronto. originally to serve third world countries.
But Chris Hall, the association's director of operations, said that a rural hospital closure in 1992 had also forced the organization to address the medical needs of under-serviced people , At her place.
"Only today, seven US states participated in this event," said Hall. "People got into their car and traveled 200 kilometers to get here today, just to be able to get a service that they could not get in their area or [couldn’t] to afford in their area. "
CBS News
Some who queued all night in the cold had a hospital; they simply did not have the insurance to access it. But for others, like Leanna Steele, it's the closest thing to an emergency room. Her local hospital, where she went when she suffered from debilitating migraines, also closed.
Cowan asked, "So, what are you doing now?"
"Above all, sit down and hope," said Steele.
Before the full closure of a hospital, administrators usually try to reduce non-urgent services, such as maternity hospitals. This has happened so often that more than half of the rural communities in the country no longer have units of labor and delivery, leaving pregnant women facing long periods of driving in the country. worst moments.
But in Lakin, Kansas, population 2,200, they tried something different. The only hospital with kilometers has instead decided to invest in obstetric care, the idea being that babies can be a growing industry. They attract patients and, as hoped the young general manager of the Kearny County Hospital Hospital, Ben Anderson, they stay … and also bring the rest of the family.
"The moms came here and had a great experience, they said:" You know, you're going to be my baby's pediatrician, you're going to be the doctor for my wife's health, and you're going to take care from my internist husband, we all come to you, "said Anderson.
CBS News
And that's just what happened. Dr. Drew Miller has a bulletin board outside his office with pictures of future patients that he has brought into this world – nearly 500 over the last eight years, coming from all the state.
"The most rewarding thing I can do is to care for families of many generations," said Dr. Miller. "I could tell you stories of people that I delivered to their babies and who took care of their grandmother or great-grandmother." That's what I like from what I can do here. "
And another thing: there are no high level specialists employed here, not even an OB-GYN. Instead, the hospital is made up entirely of physicians trained in full-spectrum family medicine. "We have determined that we only have so much money in a vital rural access hospital to cover medical staff, so it is important that everyone is trained to do the same thing. and that it is important that everyone is willing to do it equally, "Anderson said. I said.
A typical day for these rural doctors may include a colonoscopy in the operating room in the morning and removal of a skin lesion in a clinic in the afternoon. It is a flexible and dynamic approach to rural medicine that has kept the doors of hospitals open – at least for now.
"Last year, we had the first profitable year in probably two or three decades," said Anderson. "But we drive very very close, we do not have the margin for mistakes."
It is this cutting edge that hospitals like that of Pauls Valley, Oklahoma, have stayed too long. Cowan was present when General Manager Frank Avignone gathered the staff to share some news: "You can only live so long," he said. The hospital was closing immediately.
CBS News
"I'm not sure that people really understand what's going on," Avignone told Cowan. "The story must come in. People have to see the faces of the people in this community, the employees and what they have been through, people are dying because this hospital will not be open."
Back in Tonopah, Nevada, Emmy Merrow understood these risks after an extremely long drive to a hospital with Aleyna with irreversible consequences. "She fell into a crisis that lasted three hours and lasted the whole trip," she said. "So, she has brain damage, she was not breathing properly, she was losing oxygen."
"I think the audience will wonder if it is so serious and if you are so far away from a hospital and you need help virtually all the time, why not move?" Cowan asked.
"It would be great if we had the money to move," she said. "We make enough to live, but not really to save money and make the move."
As for Elaine Minges, while her husband is gone, the rural life they loved so much has disappeared, and like many people living in small towns in America, she does not know what to do.
Cowan asked, "Do you want to stay here knowing that there is no hospital?"
"My house is here," she says. "I feel my husband here."
"What do you think he would like you to do? Would he want you to stay?"
"No," she said.
For more information:
Story produced by Sari Aviv.
[ad_2]
Source link